📌 Table of Contents ⬆

How to Reduce Inflammation Naturally: 12 Evidence-Based Methods
Chronic inflammation is quietly fueling some of America's deadliest diseases — and most people have no idea it's happening inside their bodies right now. Research published in Nature Medicine estimates that 3 out of 5 people worldwide will die from an inflammation-related disease, including heart disease, stroke, cancer, and diabetes. The good news? Learning how to reduce inflammation naturally is one of the most powerful — and accessible — things you can do to protect your long-term health starting today.
For more information, see: Harvard Health: Anti-Inflammation, Cleveland Clinic: Chronic Inflammation
📌 Quick Summary
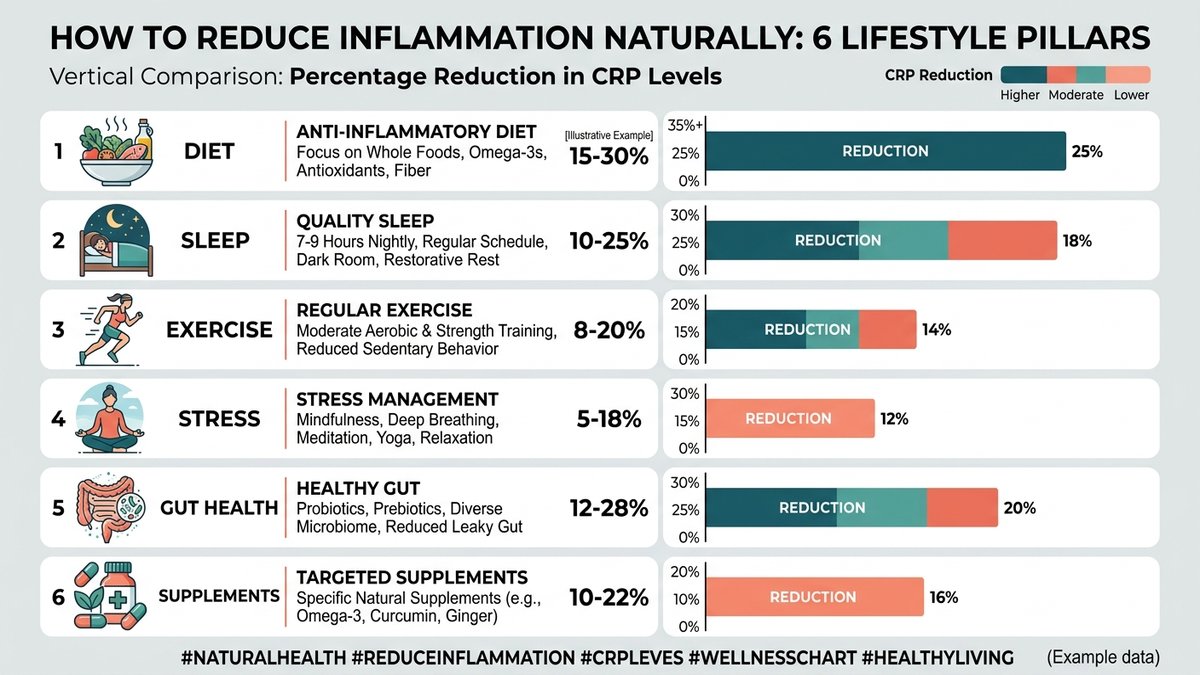
- Diet is the #1 lever: Studies show the Mediterranean diet reduces inflammatory markers like CRP by up to 20% within 3 months of adoption.
- Exercise works fast: Just 20 minutes of moderate exercise has been shown to trigger anti-inflammatory responses at the cellular level, per UC San Diego research.
- Sleep deprivation backfires: Adults sleeping fewer than 6 hours per night show significantly elevated levels of inflammatory cytokines, including IL-6 and TNF-alpha.
📊 What Is Chronic Inflammation — And Why Should You Care?
Before diving into how to reduce inflammation naturally, it's critical to understand what you're actually fighting. Inflammation itself is not the enemy — it's your immune system's built-in first responder. When you cut your finger or catch a cold, acute inflammation rushes white blood cells to the scene, speeds up healing, and then subsides. That's healthy, normal, and necessary. The problem arises with chronic low-grade inflammation, a slow-burning, persistent immune activation that operates silently in the background for months or even years. According to the Harvard T.H. Chan School of Public Health, this type of systemic inflammation is a primary driver of conditions including heart disease, type 2 diabetes, Alzheimer's disease, depression, and several cancers. What makes it particularly insidious is that you may feel perfectly fine while inflammatory damage accumulates at the cellular level — until a diagnosis suddenly appears. Understanding this distinction empowers you to take meaningful preventive action long before symptoms ever emerge.
So what triggers chronic inflammation in the first place? The list is longer than most people realize and deeply embedded in modern American lifestyles. Processed foods laden with refined sugars, industrial seed oils, and artificial additives send constant inflammatory signals to the immune system. A sedentary lifestyle allows inflammatory cytokines — chemical messengers like interleukin-6 (IL-6) and C-reactive protein (CRP) — to accumulate unchecked. Chronic psychological stress keeps the body in a constant low-level fight-or-flight state, flooding tissues with cortisol and pro-inflammatory compounds. Even gut dysbiosis — an imbalance of gut bacteria — has been directly linked to systemic inflammation through the gut-brain-immune axis. According to the Cleveland Clinic, blood tests measuring CRP levels above 3 mg/L indicate high cardiovascular risk tied to inflammation. The encouraging truth, however, is that all of these triggers are modifiable. You have far more control over your inflammatory status than most conventional medicine conversations suggest.
Anti-Inflammatory Diet
Eat whole foods to slash CRP levels naturally
Daily Movement
20 min exercise triggers powerful cell repair
Stress Reduction
Cortisol control keeps cytokines in check
| Inflammatory Trigger | Mechanism | Associated Condition | Modifiable? |
|---|---|---|---|
| Ultra-processed diet | Raises CRP, IL-6 levels | Heart disease, diabetes | Yes |
| Chronic stress | Elevates cortisol chronically | Depression, autoimmune disease | Yes |
| Poor sleep (<6 hrs) | Increases TNF-alpha, IL-6 | Obesity, cognitive decline | Yes |
| Sedentary behavior | Reduces anti-inflammatory myokines | Metabolic syndrome | Yes |
| Gut dysbiosis | Disrupts immune signaling (leaky gut) | IBD, systemic inflammation | Yes |
💡 Key takeaway: Every major trigger of chronic inflammation is lifestyle-modifiable — meaning the most powerful anti-inflammatory pharmacy may already be in your daily habits.
🎯 How to Reduce Inflammation Naturally: 12 Evidence-Based Methods
The following 12 strategies are grounded in peer-reviewed research and represent the most evidence-supported approaches to reducing inflammation naturally without relying solely on medications like NSAIDs or corticosteroids. This doesn't mean pharmaceuticals have no place — for some conditions, they are essential. But for the vast majority of Americans dealing with lifestyle-driven chronic inflammation, these natural interventions can produce measurable, lasting improvements in inflammatory biomarkers. Several of these methods work synergistically, meaning combining them amplifies the benefits beyond what any single approach can deliver. The best part? Most of them cost little to nothing and can be implemented this week. Start with one or two that feel most accessible, build consistency, and then layer in additional strategies over time. Sustainable anti-inflammatory living is a cumulative practice, not a one-time fix.
It's also worth noting that the scientific community has made enormous strides in understanding inflammation biomarkers — measurable indicators in your blood that can track your progress. Common markers include high-sensitivity C-reactive protein (hs-CRP), homocysteine, ferritin, fibrinogen, and specific interleukins. Working with a physician to baseline these numbers before beginning a natural anti-inflammatory protocol — and then retesting after 8–12 weeks — gives you objective data on what's actually working for your unique physiology. Studies consistently show that dietary changes alone can reduce hs-CRP by 20–30% within three months, while combining diet with exercise and stress management can drive even greater reductions. Think of these 12 methods as a comprehensive, personalized toolkit — not a rigid prescription.
Adopt an Anti-Inflammatory Diet
The Mediterranean diet and the MIND diet are the two most rigorously studied anti-inflammatory eating patterns. Both emphasize fatty fish (salmon, sardines, mackerel) rich in omega-3 fatty acids (EPA and DHA), colorful vegetables and fruits loaded with polyphenols and antioxidants, whole grains, legumes, nuts, and extra virgin olive oil — a source of oleocanthal, a compound with ibuprofen-like anti-inflammatory properties. A landmark 2018 study in the *New England Journal of Medicine* found that adherents of the Mediterranean diet had significantly lower levels of CRP and IL-6. Conversely, eliminate or drastically reduce ultra-processed foods, refined carbohydrates, sugar-sweetened beverages, trans fats, and excess omega-6 fatty acids from vegetable oils like corn and soybean oil, which promote the inflammatory arachidonic acid pathway. A simple rule: if it has more than five ingredients or comes in a crinkly package, think twice.
Exercise Regularly (Even Briefly)
A groundbreaking study from the University of California San Diego published in *Brain, Behavior, and Immunity* found that just 20 minutes of moderate-intensity exercise — such as brisk walking — was enough to activate the sympathetic nervous system and produce a measurable anti-inflammatory response at the cellular level, reducing TNF production by immune cells. Regular physical activity also stimulates muscles to release anti-inflammatory myokines — proteins like IL-6 (which, paradoxically, acts as an anti-inflammatory signal when produced by muscle contraction) and irisin. The CDC recommends at least 150 minutes of moderate aerobic activity per week, and research supports this target for meaningful reductions in systemic inflammation. Resistance training provides additional benefits by reducing visceral fat — a major inflammatory depot in the body. The key is consistency over intensity; daily movement beats occasional intense workouts for sustained anti-inflammatory benefits.
Prioritize Quality Sleep
Sleep is when your body performs its most critical repair and immune-regulation work — and chronic sleep deprivation is one of the fastest ways to spike inflammatory markers. A study published in *Sleep* journal found that adults restricted to 6 hours of sleep per night for just one week showed significantly elevated levels of IL-6, TNF-alpha, and CRP compared to those sleeping 7–9 hours. The National Sleep Foundation recommends 7–9 hours nightly for adults, yet the CDC reports that more than 1 in 3 Americans regularly fall short of this target. Poor sleep quality — not just duration — matters too; fragmented sleep disrupts the glymphatic system (the brain's waste-clearance network) and impairs cortisol regulation. Practical strategies to improve sleep quality include maintaining a consistent sleep-wake schedule, keeping your bedroom cool and dark, avoiding blue light exposure from screens 90 minutes before bed, and limiting caffeine after 2 PM.
Manage Stress with Mind-Body Practices
Chronic psychological stress is one of the most underappreciated drivers of systemic inflammation in America today. When the brain perceives a threat — whether real or imagined — it triggers the hypothalamic-pituitary-adrenal (HPA) axis, flooding the body with cortisol and adrenaline. In acute situations, this is adaptive. But when stress is chronic, sustained cortisol elevation promotes the production of pro-inflammatory cytokines and impairs the immune system's ability to regulate itself. Mindfulness-Based Stress Reduction (MBSR), an 8-week structured program developed at UMass Medical School, has been shown in multiple randomized controlled trials to reduce CRP and IL-6 levels, improve immune function, and even alter gene expression related to inflammation. Other evidence-supported practices include yoga, tai chi, diaphragmatic breathing, and progressive muscle relaxation. Even 10 minutes of daily mindfulness meditation, as studied in research from Carnegie Mellon University, measurably reduces inflammatory markers over time.
⚖️ Natural Anti-Inflammatory Supplements: What the Evidence Actually Says
The supplement market is flooded with products claiming to fight inflammation, but the scientific evidence behind them varies wildly. Some natural anti-inflammatory supplements have robust clinical trial data supporting their effectiveness; others are based on preliminary or in vitro (lab dish) research that hasn't translated reliably to human outcomes. It's important to approach supplementation with a discerning eye — and always consult a healthcare provider before adding anything new, especially if you take prescription medications. That said, several supplements stand out for their quality of evidence. Curcumin (the active compound in turmeric) has been evaluated in over 120 clinical trials, with multiple studies showing significant reductions in CRP, IL-6, and NF-κB — a master regulator of inflammatory gene expression. Fish oil (omega-3s) is arguably the most researched natural anti-inflammatory compound available, with the American Heart Association endorsing omega-3 supplementation for people with existing heart disease. Magnesium deficiency — affecting an estimated 48% of Americans according to the National Institutes of Health — is directly associated with elevated CRP levels, making magnesium supplementation a surprisingly impactful intervention for many people.
Understanding the difference between supplements that modestly support an already healthy lifestyle and those that can serve as meaningful therapeutic tools is key. Resveratrol, found in red wine and grape skin, shows anti-inflammatory promise in laboratory and some human studies — but bioavailability remains a challenge, meaning the body doesn't always absorb it efficiently in standard oral forms. Vitamin D deficiency, affecting roughly 42% of American adults per research in Nutrition Research, is strongly associated with elevated inflammatory markers, and supplementation in deficient individuals consistently reduces them. Probiotics represent one of the most exciting frontiers: specific strains like Lactobacillus rhamnosus GG and Bifidobacterium longum have demonstrated the ability to reduce gut-derived inflammation and lower systemic cytokine levels in clinical trials. The bottom line: supplements can be powerful adjuncts to a natural anti-inflammatory lifestyle, but they work best when built on a foundation of whole-food nutrition, regular movement, and restorative sleep — not as shortcuts in their absence.
Pros
- ✅ Curcumin + black pepper (piperine): Increases curcumin bioavailability by up to 2,000%, with trials showing 30%+ reduction in CRP in inflammatory conditions
- ✅ Omega-3 fatty acids (EPA/DHA): Directly resolve inflammation via specialized pro-resolving mediators (SPMs); widely supported by AHA guidelines
- ✅ Magnesium glycinate: Corrects widespread deficiency linked to elevated CRP; also improves sleep quality, amplifying anti-inflammatory benefits
- ✅ Vitamin D3 + K2: Restores deficiency in 42% of Americans; D3 regulates immune response and reduces inflammatory cytokine production
Cons
- ❌ Drug interactions are real: Fish oil at high doses can increase bleeding risk; curcumin may interfere with blood thinners like warfarin — always consult your doctor
- ❌ Supplement quality is unregulated: The FDA doesn't evaluate supplements before sale; look for USP, NSF, or Informed Sport certifications to ensure purity and potency
- ❌ No supplement replaces lifestyle: Even the best-evidenced supplements provide modest benefits compared to the combined impact of diet, exercise, sleep, and stress management
⚠️ Important warning: If you have an autoimmune condition, are pregnant, or take prescription blood thinners, immunosuppressants, or anti-inflammatories, consult your physician before starting any anti-inflammatory supplement regimen. Natural does not automatically mean safe for every individual.
✅ Additional Lifestyle Methods to Reduce Inflammation Naturally (Methods 5–12)
Beyond diet, exercise, sleep, and stress management, several additional evidence-based lifestyle strategies meaningfully reduce chronic inflammation. Intermittent fasting (IF) — particularly the 16:8 time-restricted eating model — has been shown in a 2019 study published in *Cell Metabolism* to reduce inflammatory markers including IL-6 and CRP, partly by inducing autophagy (cellular self-cleaning) and reducing visceral fat. Quitting smoking is non-negotiable: cigarette smoke contains thousands of oxidants and pro-inflammatory compounds, and the CDC confirms that smoking is a primary independent driver of systemic inflammation and accelerated aging. Reducing alcohol consumption also matters significantly — while a small amount of red wine may have mild anti-inflammatory polyphenols, heavy drinking dramatically elevates CRP and disrupts gut barrier integrity, promoting what researchers call leaky gut syndrome. Staying well-hydrated supports kidney function and the removal of inflammatory metabolic waste products; the National Academies of Sciences recommends approximately 3.7 liters of total daily water intake for men and 2.7 liters for women. Spending time in nature (forest bathing) — a practice studied extensively in Japan as *Shinrin-yoku* — has been shown to reduce cortisol levels by up to 12.4% and lower blood pressure and inflammatory markers after just 15 minutes outdoors. These aren't fringe wellness trends; they're backed by solid science.
Three additional methods round out the picture. Cold water therapy — including cold showers or brief cold-water immersion — activates the vagus nerve and triggers a norepinephrine surge that powerfully suppresses inflammatory cytokine production. Research from the Wim Hof Method studies published in *PNAS* showed that trained individuals could voluntarily suppress immune system activation and reduce inflammatory markers through combined breathing and cold exposure techniques. Reducing exposure to environmental toxins is equally important: endocrine-disrupting chemicals (EDCs) like BPA in plastics, phthalates in personal care products, and pesticide residues in non-organic produce have all been linked to elevated inflammatory signaling. Choosing glass or stainless steel food storage, selecting fragrance-free personal care products, and prioritizing the EWG's Clean Fifteen produce list are practical ways to reduce your body's toxic burden. Finally, nurturing meaningful social connections — frequently overlooked in discussions of inflammation — is supported by research from Brigham Young University showing that social isolation increases inflammatory markers comparably to smoking 15 cigarettes per day. Humans are fundamentally social animals, and our immune systems know it.
❓ Frequently Asked Questions
✍️ Final Thoughts: Your Next Step Toward a Less Inflamed Life
Chronic inflammation doesn't have to be your destiny. The science is unambiguous: the most powerful tools for reducing inflammation naturally are the ones embedded in your daily choices — the food on your plate, the hours you spend moving, the quality of your sleep, the way you manage stress, and the connections you nurture with other people. We've covered 12 evidence-based methods, from adopting a Mediterranean-style anti-inflammatory diet and exercising for as little as 20 minutes a day, to optimizing sleep hygiene, practicing mindfulness, selecting the right supplements, and even reducing your exposure to environmental toxins. Each of these strategies is supported by peer-reviewed research — not wellness influencers or marketing copy. And crucially, they work synergistically: the more you stack them together, the greater your reduction in systemic inflammatory markers like hs-CRP, IL-6, and TNF-alpha. You don't have to overhaul your entire life overnight. Start with the two or three strategies that feel most accessible and build momentum from there. Small, consistent changes compound dramatically over weeks, months, and years into profoundly different health outcomes.
Here's your action plan for this week: First, make an appointment with your doctor to request a baseline hs-CRP and vitamin D blood test — you can't manage what you don't measure. Second, audit your kitchen and remove the three biggest inflammatory offenders in your diet: sugar-sweetened beverages, refined vegetable oils (corn, soybean, canola), and ultra-processed snack foods. Replace them with wild-caught salmon, extra virgin olive oil, and a handful of walnuts. Third, commit to a 20-minute walk every day this week — not because it sounds impressive, but because science confirms it's enough to meaningfully shift your body's inflammatory chemistry. Fourth, choose one stress-reduction practice — even five minutes of deep breathing each morning — and do it every day for two weeks straight. Track how you feel. The anti-inflammatory journey is not about perfection; it's about consistent, informed progress. Your immune system is remarkably responsive to the right inputs, and the body you're living in right now has enormous capacity to heal when given what it needs. Visit InfoWellHub.com for more evidence-based health guidance, and remember: every meal, every walk, every good night's sleep is a vote for a less inflamed, healthier version of yourself.
Post a Comment