📌 Table of Contents ⬆

Omega 3 Side Effects: What Your Doctor May Not Tell You
Omega 3 side effects are something millions of Americans experience every day — yet most people pop their fish oil capsule each morning without a second thought. With over 20 million U.S. adults taking omega-3 supplements regularly, it's shocking how little conversation happens about the real downsides. Whether you're dealing with fishy burps, unexpected bruising, or wondering if your daily dose is quietly raising your blood sugar, this guide covers everything your doctor may not have mentioned — backed by science, not guesswork.
For more information, see: NIH Office of Dietary Supplements — Omega-3 Fatty Acids Fact Sheet, InfoWellHub — Daily Vitamins and Supplements Guide
📌 Quick Summary
- Gastrointestinal upset is the #1 complaint: Studies show up to 30% of omega-3 users report bloating, nausea, or fishy burps — especially with low-quality supplements taken on an empty stomach.
- Bleeding risk is real and underreported: High-dose omega-3s (above 3,000 mg/day) can inhibit platelet aggregation, increasing bleeding time — a serious concern for anyone on blood thinners like warfarin.
- Dose matters more than most labels admit: The FDA considers up to 3,000 mg/day of EPA+DHA from supplements to be generally safe, but many popular products contain far more than users realize when stacked together.
📊 The Most Common Omega 3 Side Effects You Should Know
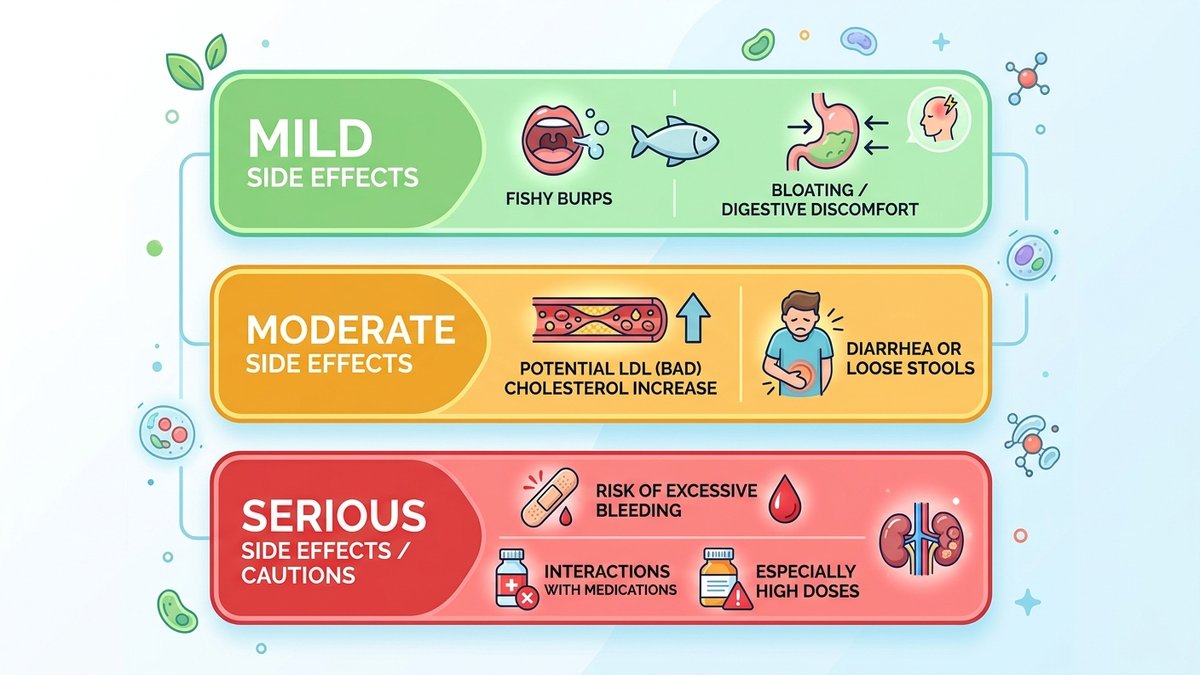
Omega 3 side effects range from mildly annoying to genuinely medically significant, and understanding the full spectrum is the first step to supplementing safely. The most frequently reported issue is gastrointestinal discomfort — including fishy burps, nausea, loose stools, and bloating. This is especially true with the classic fish oil capsule form, where the oil can oxidize quickly, producing that notorious 'repeat' sensation hours after swallowing. Research published in the *American Journal of Clinical Nutrition* found that up to 30% of regular fish oil users experience some form of GI disturbance. Interestingly, enteric-coated capsules and algae-based omega-3s tend to produce significantly fewer digestive complaints, suggesting the issue is as much about formulation as it is about the nutrient itself. If you've ever blamed your supplement and quit, you likely just had the wrong format — not the wrong nutrient.
Beyond the gut, fish oil adverse effects can include headaches, bad breath, and an unpleasant taste that lingers throughout the day. Less talked about are the cardiovascular nuances: while omega-3s are celebrated for lowering triglycerides, very high doses — think above 4,000–5,000 mg EPA+DHA daily — have been associated with modest increases in LDL ('bad') cholesterol in some individuals, particularly those with existing lipid disorders. A 2021 meta-analysis in the *Journal of the American Heart Association* noted this paradox and urged personalized dosing. Additionally, vitamin A toxicity is a concern specific to cod liver oil supplements, which contain preformed vitamin A alongside omega-3s. Consistently exceeding safe vitamin A limits can lead to bone pain, liver damage, and birth defects in pregnancy — a serious risk often buried in the fine print of cod liver oil labels.
Fishy Burps & Bloating
Most common omega 3 side effect — affects up to 30% of users
Bleeding Risk Warning
High doses thin blood — critical if you take medications
Blood Sugar Spike Risk
Very high doses may modestly raise LDL and blood glucose
| Side Effect | Estimated Prevalence | Severity Level | Who Is Most at Risk |
|---|---|---|---|
| Fishy burps / reflux | Up to 30% of users | Mild | Anyone using non-enteric-coated fish oil |
| Nausea & loose stools | 10–15% of users | Mild–Moderate | Those taking on an empty stomach |
| Increased bleeding time | Dose-dependent | Moderate–Serious | People on blood thinners or pre-surgery |
| LDL cholesterol increase | Seen at >4,000 mg/day | Moderate | Those with existing lipid disorders |
| Vitamin A toxicity | Rare (cod liver oil only) | Serious | Pregnant women, high-dose users |
💡 Key takeaway: Most omega 3 side effects are dose-dependent and formulation-dependent — switching to enteric-coated or algae-based options eliminates the majority of GI complaints for most users.
🎯 Omega 3 Side Effects Fish Oil Bloating and Burping: How to Fix It
The dreaded omega 3 side effects of fish oil bloating and burping are by far the most universal complaint — and ironically, the most avoidable. The core issue is oxidation: when fish oil is poorly processed or stored, the delicate fatty acids (EPA and DHA) break down into rancid compounds that not only smell and taste terrible but also irritate the gastrointestinal lining. Studies testing popular fish oil brands found that a significant portion of retail products showed signs of oxidation exceeding international freshness standards, even before their expiration date. This means that the 'fishy burp' problem isn't just unpleasant — it may signal that your supplement has already degraded and lost much of its therapeutic value. Before assuming omega-3s simply 'don't agree with you,' it's worth auditing the quality and storage method of your supplement first.
The good news is that a few practical strategies dramatically reduce or eliminate these omega 3 side effects. Timing is everything: taking your supplement with your largest meal slows digestion and prevents the oil from sitting alone in your stomach. Refrigerating your capsules slows oxidation and reduces odor. Choosing enteric-coated capsules means they dissolve in the small intestine rather than the stomach, virtually eliminating burping and reflux for most people. Alternatively, switching to algae-based omega-3 supplements — the original plant-based source that fish eat to produce their EPA and DHA — bypasses the fish entirely, producing no fishy smell and causing far fewer GI issues in clinical comparisons. Many gastroenterologists now recommend the algae route as the first-line choice for sensitive stomachs.
Switch to Enteric-Coated Capsules
Enteric coating is a pharmaceutical technique that prevents the capsule from dissolving in the acidic stomach environment and instead releases the oil in the more neutral small intestine. This single change eliminates fishy burps for the vast majority of users because the oil never has a chance to produce gas or reflux in the upper digestive tract. Look for supplements specifically labeled 'enteric coated' or 'delayed release' — they cost slightly more but represent one of the most effective solutions to the omega 3 side effects of bloating and burping. Multiple consumer trials have confirmed this approach reduces GI complaints by over 50% compared to standard softgels.
Always Take with Food
Taking omega-3 supplements on an empty stomach is one of the most common mistakes users make. Without food present, the stomach empties rapidly and the oil can sit in the upper GI tract, ferment slightly, and cause nausea, belching, and discomfort. Taking your dose with your biggest meal of the day — ideally one that contains some dietary fat — slows gastric emptying, helps emulsify the omega-3 oil, and dramatically reduces the likelihood of any digestive fish oil adverse effects. Clinical guidance consistently recommends food co-administration as the simplest, free-of-cost intervention for GI tolerance.
Refrigerate Your Fish Oil
Oxidation is the enemy of fish oil quality and one of the root causes of GI side effects. Once a bottle is opened, exposure to light, heat, and air rapidly degrades the fragile EPA and DHA fatty acids. Storing your fish oil in the refrigerator — even if the label doesn't require it — significantly slows this process and preserves freshness. You can also do a quick freshness test: cut open a capsule and smell it. Fresh fish oil should smell like the ocean, mildly. If it smells strongly rancid or 'off,' discard the bottle immediately — oxidized oil offers little benefit and may contribute to inflammation rather than reducing it.
Consider Algae-Based Omega-3s
Algae-derived omega-3 supplements are the plant-based alternative that is rapidly gaining favor among nutritionists, vegans, and anyone with a sensitive digestive system. Since fish obtain their EPA and DHA by consuming microalgae, going directly to the source produces a supplement that is molecularly equivalent — without the fishy smell, oxidation risk, or environmental concerns of fish harvesting. Multiple clinical studies have confirmed that algae-based DHA is absorbed as effectively as fish oil DHA. Brands like Ovega-3 and Nordic Naturals Algae Omega have demonstrated clean tolerance profiles with dramatically fewer GI complaints in user surveys. This is particularly relevant for pregnant women who need DHA but are cautious about fish-sourced products.
⚖️ Can Omega 3 Cause Bleeding Risk with Blood Thinners? The Real Answer
One of the most clinically significant and underappreciated omega 3 side effects is the potential to increase bleeding risk, particularly for people already taking anticoagulant or antiplatelet medications. Omega-3 fatty acids — especially EPA — have well-documented anti-platelet properties, meaning they reduce the stickiness of platelets and can prolong bleeding time. At moderate doses (under 2,000 mg EPA+DHA per day), this effect is generally mild and even considered beneficial for cardiovascular health in otherwise healthy adults. However, when combined with medications like warfarin (Coumadin), aspirin, clopidogrel (Plavix), or direct oral anticoagulants like apixaban (Eliquis), the combined effect can push bleeding risk to clinically dangerous levels. A 2019 review in *Thrombosis and Haemostasis* flagged this interaction as significantly underreported in primary care settings.
The concern around 'can omega 3 cause bleeding risk with blood thinners' is not theoretical — it has real-world consequences. There are documented case reports of patients experiencing excessive bruising, prolonged nosebleeds, and heightened surgical bleeding risk when combining high-dose omega-3 supplements with blood-thinning medications without physician oversight. The American Heart Association recommends that patients on anticoagulants inform their cardiologist or internist before starting or increasing omega-3 supplementation. It's also worth noting that pre-surgical patients are routinely advised to stop fish oil 1–2 weeks before any procedure precisely because of this platelet-inhibiting effect. The bottom line: omega-3s and anticoagulants can coexist safely under medical supervision, but the combination demands active monitoring.
Pros
- ✅ Triglyceride reduction: Prescription omega-3s (Vascepa, Lovaza) are FDA-approved to reduce triglycerides by up to 45% in high-risk patients
- ✅ Anti-inflammatory benefits: EPA and DHA modulate inflammatory pathways, reducing markers like CRP and IL-6 in multiple clinical trials
- ✅ Cardiovascular support: The REDUCE-IT trial showed icosapentaenoic acid (EPA) reduced major cardiovascular events by 25% vs. placebo
- ✅ Brain and mood health: DHA is a structural component of neuronal membranes, with studies linking adequate intake to lower rates of depression and cognitive decline
Cons
- ❌ Bleeding risk amplification: High doses combined with anticoagulants can dangerously prolong clotting time — requires medical supervision
- ❌ LDL cholesterol paradox: Doses above 4,000 mg/day may modestly raise LDL in some individuals, counteracting cardiovascular intent
- ❌ Vitamin A toxicity risk (cod liver oil): Excessive cod liver oil intake can cause vitamin A accumulation, leading to liver damage and bone fragility over time
⚠️ Important warning: If you are taking any blood-thinning medication — including daily aspirin — always tell your doctor before starting omega-3 supplementation above 1,000 mg/day. The interaction between omega-3s and anticoagulants is real, clinically documented, and requires active monitoring to stay safe.
✅ How Much Omega 3 Is Too Much Per Day — and How to Dose Safely
Understanding how much omega 3 is too much per day is arguably the most important piece of knowledge for any supplement user — and one that most product labels obscure rather than clarify. The FDA considers up to 3,000 mg of EPA+DHA per day from dietary supplements to be generally recognized as safe (GRAS) for healthy adults. The European Food Safety Authority (EFSA) sets a slightly more generous limit of 5,000 mg/day for long-term supplementation in adults, citing no evidence of harm at that threshold in clinical trials. However, 'no evidence of harm' is not the same as 'optimal,' and most research on cardiovascular and anti-inflammatory benefits uses doses in the 1,000–3,000 mg EPA+DHA range. The disconnect between 'total omega-3' labeled on the front of a bottle and 'actual EPA+DHA content' buried in the supplement facts panel is one of the most persistent consumer traps in the supplement industry — a bottle labeled '2,000 mg omega-3' may only contain 600 mg of combined EPA+DHA, with the rest being other fatty acids. Always read the supplement facts panel, not the front-of-label claim. You can explore more about safe supplement dosing in our guide to [choosing the right daily vitamins and supplements](https://infowellhub.com/daily-vitamins-and-supplements-guide).
For practical, day-to-day supplementation, the American Heart Association recommends 1,000 mg of EPA+DHA per day for people with documented coronary heart disease, and suggests that people without cardiovascular disease simply eat two servings of fatty fish (salmon, mackerel, sardines) per week as their primary omega-3 source. If you're supplementing for general wellness, most integrative medicine physicians land in the 500–1,000 mg EPA+DHA daily range as a safe, evidence-based sweet spot that avoids the omega 3 side effects associated with higher doses. If you're considering prescription-strength omega-3 therapy — such as Vascepa (icosapentaenoic acid) at 4 grams/day — that must be done under physician supervision with regular lipid panel monitoring. The key action for anyone supplementing is to calculate your actual EPA+DHA intake across all sources (supplements, fortified foods, fish consumption), not just assume the label total represents therapeutic omega-3. For authoritative guidance on safe supplementation, the [NIH Office of Dietary Supplements omega-3 fact sheet](https://ods.od.nih.gov/factsheets/Omega3FattyAcids-HealthProfessional/) provides comprehensive, regularly updated evidence summaries.
❓ Frequently Asked Questions
✍️ Final Thoughts: Your Next Step with Omega 3 Supplements
Omega 3 side effects are real, documented, and more nuanced than most supplement labels — or doctors' appointments — let on. The good news is that the vast majority of people can enjoy the well-established cardiovascular, anti-inflammatory, and cognitive benefits of omega-3 supplementation by simply being informed and intentional. The biggest culprits behind bad experiences are poor supplement quality, incorrect dosing, and failure to account for medication interactions. Fishy burps and bloating — the most common complaints — are almost entirely preventable through enteric-coated formulations, meal-time dosing, and proper storage. Bleeding risk is a genuine clinical concern, but it becomes manageable under medical supervision rather than a reason to avoid omega-3s altogether. And for anyone asking how much omega 3 is too much per day, the answer is clear: stay below 3,000 mg EPA+DHA daily from supplements without medical guidance, and always read the supplement facts panel to understand what you're actually getting. Fish oil adverse effects at appropriate doses in healthy adults are mild and manageable — the risk-benefit equation remains strongly favorable for most people.
So what should you do right now? Start with three action steps. First, pull out your current omega-3 supplement and flip it over — check the supplement facts panel for the actual EPA+DHA milligrams, not the total omega-3 figure on the front. Second, if you're on any prescription medication — especially blood thinners, cholesterol drugs, or diabetes medications — bring your omega-3 supplement to your next doctor's appointment and ask specifically about interactions. Third, if you've quit omega-3 supplements in the past due to fishy burps or stomach upset, try an enteric-coated or algae-based alternative for 30 days before writing off the category entirely. The supplement form makes an enormous difference in tolerance. For the most up-to-date clinical guidance on omega-3 supplementation, bookmark the [NIH Office of Dietary Supplements omega-3 fact sheet](https://ods.od.nih.gov/factsheets/Omega3FattyAcids-HealthProfessional/) — it's updated regularly as new research emerges and is the gold standard for evidence-based supplementation decisions. Your health deserves both the benefits and the full picture.
Post a Comment