📌 Table of Contents ⬆

How to Reduce Inflammation Naturally: 12 Evidence-Based Methods
Chronic inflammation is now recognized as a silent driver behind some of America's deadliest diseases — including heart disease, type 2 diabetes, Alzheimer's, and certain cancers. According to the CDC, 6 in 10 American adults live with at least one chronic disease, many of which are directly linked to persistent, low-grade inflammation. If you've been wondering how to reduce inflammation naturally, the science has never been clearer — and the solutions are more accessible than you might think.
For more information, see: Harvard Health: Anti-Inflammation, Cleveland Clinic: Chronic Inflammation
📌 Quick Summary
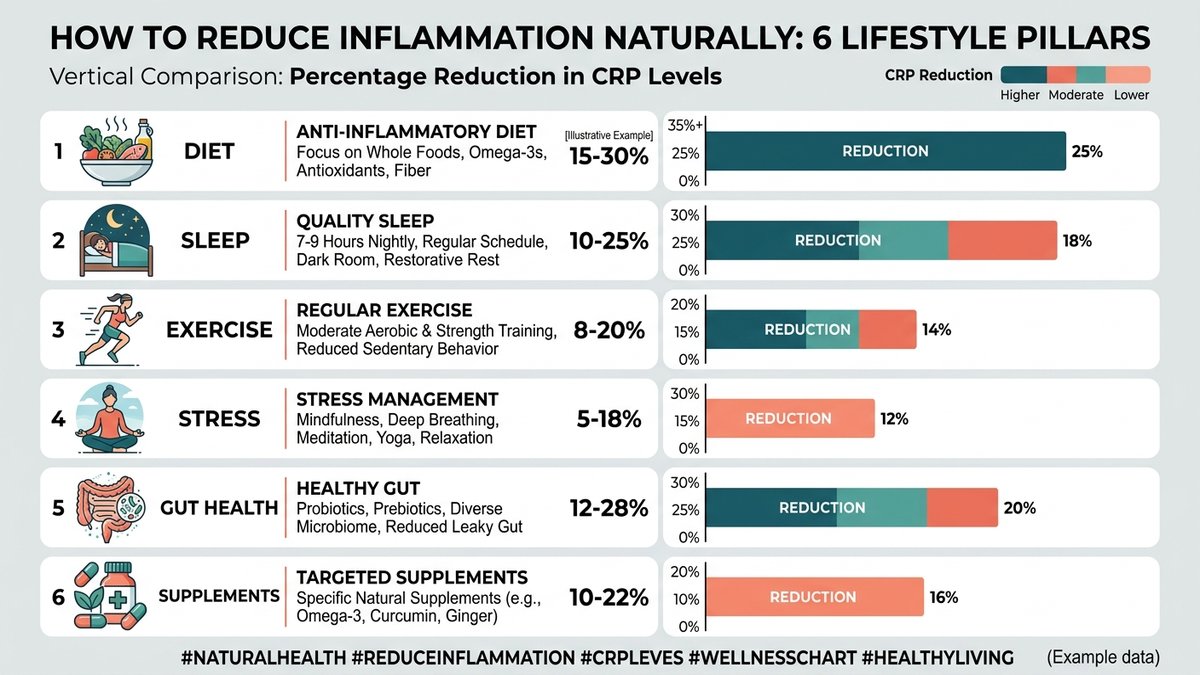
- Diet is the #1 lever: Studies show the Mediterranean diet reduces inflammatory markers like CRP by up to 20% within 3 months of consistent adherence.
- Sleep deprivation spikes inflammation: Even one night of poor sleep can elevate pro-inflammatory cytokines like IL-6 and TNF-alpha, according to research published in *Sleep* journal.
- Exercise works fast: A single 20-minute session of moderate aerobic exercise has been shown to produce anti-inflammatory effects by activating the sympathoadrenergic mechanism in immune cells.
📊 Understanding Inflammation: What the Science Actually Says
Before diving into how to reduce inflammation naturally, it's essential to understand what inflammation actually is — and why not all of it is bad. Acute inflammation is your body's healthy, short-term response to injury or infection. When you sprain your ankle or catch a cold, your immune system dispatches white blood cells and chemical messengers called cytokines to the affected area, triggering redness, swelling, and heat. This process is critical for healing and typically resolves within a few days. The real danger lies in chronic inflammation — a state where your immune system remains in a low-grade, persistent state of alarm even when there's no immediate threat. Over months and years, this constant cellular stress damages tissues, disrupts hormonal signaling, and contributes to the development of serious diseases. Research published in *Nature Medicine* confirms that chronic inflammatory diseases are the most significant cause of death worldwide, accounting for more than 50% of all deaths globally.
The tricky part about chronic inflammation is that it's largely invisible. Most people don't feel inflamed — they just feel tired, foggy, achy, or generally unwell. Biomarkers like C-reactive protein (CRP), interleukin-6 (IL-6), and tumor necrosis factor-alpha (TNF-α) are the tools doctors use to detect inflammation in the bloodstream, but routine checkups don't always include these tests. A 2022 analysis published in *The Lancet* found that millions of Americans have elevated inflammatory markers without knowing it. Lifestyle choices — including a poor diet, physical inactivity, chronic stress, inadequate sleep, and environmental toxin exposure — are the primary fuels feeding this fire. The good news is that these same lifestyle factors are the most powerful levers you can pull to turn it off. Every method in this guide is backed by peer-reviewed research and designed to be practical for real Americans navigating real, busy lives.
Anti-Inflammatory Diet
Eat your way to lower CRP and IL-6 levels
Quality Sleep
7–9 hrs nightly resets your immune response
Regular Exercise
20 min of movement cuts cytokine levels fast
| Inflammation Type | Duration | Key Drivers | Health Impact |
|---|---|---|---|
| Acute (Healthy) | Days to weeks | Injury, infection, surgery | Essential for healing |
| Chronic (Harmful) | Months to years | Poor diet, stress, inactivity | Heart disease, diabetes, cancer |
| Metabolic Inflammation | Ongoing | Obesity, high-sugar diet | Insulin resistance, fatty liver |
| Neuroinflammation | Long-term | Sleep loss, stress, trauma | Depression, Alzheimer's risk |
| Autoimmune Inflammation | Persistent | Genetic + environmental triggers | RA, lupus, IBD, MS |
💡 Key takeaway: Chronic inflammation is largely lifestyle-driven — which means it's also largely lifestyle-reversible with the right, consistent habits.
🎯 12 Evidence-Based Methods to Reduce Inflammation Naturally
The following methods are not wellness trends or social media fads — they are strategies validated by clinical trials, meta-analyses, and decades of nutritional and physiological research. Learning how to reduce inflammation naturally requires a multi-pronged approach because inflammation is influenced by nearly every system in your body: your gut, your hormones, your nervous system, and your immune system all play interconnected roles. Addressing just one area will help, but combining several of these strategies creates a compounding effect that researchers describe as a synergistic anti-inflammatory lifestyle. The most powerful changes are often the simplest ones, and many of them cost nothing at all. What they do require is consistency — inflammation didn't build up overnight, and it won't resolve overnight either. Most studies show measurable improvements in inflammatory biomarkers within 4 to 12 weeks of sustained lifestyle change, which is genuinely fast when you consider the decades it took for many chronic conditions to develop.
Think of this list as your personalized toolkit. You don't have to implement all 12 methods at once — in fact, research on behavior change suggests that starting with 2 to 3 high-impact habits and building from there leads to far better long-term adherence than overhauling everything simultaneously. Prioritize the methods that align most closely with your current lifestyle gaps. If you're sleeping poorly, start with sleep. If your diet is heavy in processed foods, start there. The beauty of an anti-inflammatory lifestyle is that each positive change tends to reinforce the others: better sleep improves dietary choices, exercise reduces stress, and a healthier gut supports more restful sleep. This guide is designed to give you enough scientific context to understand *why* each strategy works, and enough practical guidance to actually implement it starting today.
Adopt an Anti-Inflammatory Diet
The Mediterranean diet is the most rigorously studied anti-inflammatory eating pattern in the world, with hundreds of clinical trials supporting its benefits. Rich in extra-virgin olive oil, fatty fish, leafy greens, legumes, nuts, and colorful vegetables, this dietary pattern consistently lowers CRP, IL-6, and other inflammatory markers. A landmark meta-analysis published in *Nutrients* (2019) found that adherence to the Mediterranean diet was associated with a significant reduction in CRP levels across 17 randomized controlled trials. Key foods to prioritize include wild-caught salmon (rich in omega-3 fatty acids), turmeric (curcumin content), blueberries (anthocyanins), leafy greens (vitamin K and polyphenols), and olive oil (oleocanthal). Foods to minimize include refined sugars, white flour, processed seed oils like soybean and corn oil, and ultra-processed packaged snacks — all of which have been shown to spike inflammatory cytokines within hours of consumption.
Prioritize 7–9 Hours of Quality Sleep
Sleep is one of the most underrated anti-inflammatory tools available to you — and it's free. During deep sleep, your body downregulates the production of pro-inflammatory cytokines and ramps up cellular repair processes. Research from the University of California, Berkeley demonstrated that even one night of sleep deprivation causes a measurable increase in inflammatory gene expression and raises levels of IL-6 and TNF-alpha the following day. Chronic short sleepers — those averaging fewer than 6 hours per night — have been shown in multiple studies to have significantly higher CRP levels than those who sleep 7–9 hours. To improve sleep quality, focus on maintaining a consistent bedtime, keeping your bedroom cool (around 65–68°F is ideal), eliminating blue light exposure from screens at least 60 minutes before bed, and avoiding caffeine after 2 PM. Magnesium glycinate (200–400 mg) taken before bed has also been clinically shown to improve sleep quality and may independently reduce inflammation.
Exercise Regularly — But Don't Overdo It
Physical activity is one of the most powerful and immediate anti-inflammatory interventions known to science. A 2017 study published in Brain, Behavior, and Immunity found that just 20 minutes of moderate-intensity aerobic exercise — enough to raise your heart rate — triggered a sympathoadrenergic response that suppressed the production of TNF-alpha by up to 5%. Over the long term, regular exercise reduces visceral fat (a major source of inflammatory cytokines), improves insulin sensitivity, and lowers resting CRP levels. The sweet spot appears to be 150–300 minutes of moderate aerobic activity per week, as recommended by the American Heart Association, combined with 2 days of strength training. However, it's equally important to note that excessive, high-intensity exercise without adequate recovery can actually spike inflammation — a phenomenon well-documented in overtraining syndrome. Balance is key: consistent, moderate movement beats sporadic, brutal workouts every time.
Manage Chronic Stress with Mind-Body Practices
Chronic psychological stress is a major driver of inflammation that most people dramatically underestimate. When you're stressed, your hypothalamic-pituitary-adrenal (HPA) axis releases cortisol — a hormone that, in short bursts, is actually anti-inflammatory. But when cortisol is chronically elevated due to ongoing stress, your immune cells develop cortisol resistance, causing them to over-produce inflammatory cytokines like IL-6 and IL-1β. A comprehensive 2014 meta-analysis in *Psychosomatic Medicine* found that mindfulness-based stress reduction (MBSR) programs consistently lowered CRP and other inflammatory markers in chronically stressed adults. Practices with strong evidence include mindfulness meditation (even 10–15 minutes daily using apps like Headspace or Calm), yoga (specifically shown to reduce IL-6 and CRP in multiple RCTs), deep diaphragmatic breathing (activates the vagus nerve and parasympathetic response), and spending time in nature — a practice Japanese researchers call *Shinrin-yoku* or forest bathing, shown to lower cortisol and NK cell activity within hours.
⚖️ Natural vs. Pharmaceutical Approaches to Inflammation: Honest Pros & Cons
When people ask how to reduce inflammation naturally, they're often asking in contrast to pharmaceutical options — NSAIDs like ibuprofen and naproxen, corticosteroids like prednisone, or newer biologics like adalimumab (Humira). These medications absolutely have their place, especially in acute situations or severe autoimmune conditions where inflammation must be controlled quickly and decisively. However, relying on pharmaceuticals as a first-line, long-term strategy for lifestyle-driven chronic inflammation comes with significant trade-offs. Long-term NSAID use is associated with a 2–3x increased risk of gastrointestinal bleeding, kidney damage, and cardiovascular events according to the FDA's own safety communications. Corticosteroids, while effective, can cause bone density loss, immune suppression, metabolic dysregulation, and adrenal suppression with extended use. For many Americans dealing with low-grade chronic inflammation driven by modifiable lifestyle factors, the risk-benefit analysis increasingly favors natural interventions — especially when those interventions have their own robust evidence base.
That said, intellectual honesty demands acknowledging the real limitations of natural approaches. Lifestyle changes take time — typically weeks to months before significant reductions in inflammatory biomarkers are measurable — whereas an NSAID can reduce pain and swelling within hours. Natural supplements like curcumin, omega-3s, and boswellia have meaningful research behind them, but their bioavailability and dosing can be inconsistent, and the supplement industry in the US is not subject to the same rigorous pre-market testing as pharmaceutical drugs. The optimal approach for most people is an integrative one: use lifestyle and natural strategies as the foundation of your anti-inflammatory protocol, lean on evidence-based supplements when appropriate, and reserve pharmaceutical interventions for situations where they are genuinely medically necessary — always in consultation with your physician. The goal is not to reject medicine but to reduce your dependence on it by addressing root causes rather than symptoms alone.
Pros
- ✅ No serious side effects: Natural lifestyle interventions like diet, exercise, and sleep carry virtually no risk of organ damage or dependency when implemented appropriately.
- ✅ Addresses root causes: Unlike anti-inflammatory drugs that suppress symptoms, lifestyle changes target the upstream drivers — poor diet, inactivity, stress — that generate chronic inflammation in the first place.
- ✅ Compounding health benefits: Anti-inflammatory habits simultaneously improve cardiovascular health, mental health, metabolic function, and longevity — no drug delivers benefits this broad.
- ✅ Cost-effective: Most natural anti-inflammatory strategies are free or low-cost, making them accessible to the vast majority of Americans regardless of insurance status.
Cons
- ❌ Slower onset of action: Natural methods typically require 4–12 weeks of consistency before measurable reductions in inflammatory biomarkers occur — not suitable for acute inflammatory emergencies.
- ❌ Requires sustained behavioral change: The most powerful natural interventions demand consistent lifestyle shifts that many people find difficult to maintain long-term without structured support.
- ❌ Supplement quality varies widely: The US supplement industry is loosely regulated; products claiming anti-inflammatory benefits may contain inconsistent doses or undisclosed additives.
⚠️ Important warning: Never discontinue a prescribed anti-inflammatory medication in favor of natural methods without first consulting your physician. Natural approaches work best as complements to — not unilateral replacements for — medically necessary treatment plans.
✅ The 8 Additional Natural Inflammation-Fighters You Shouldn't Overlook
Beyond the four core strategies above, there are eight additional evidence-backed methods that can meaningfully accelerate your anti-inflammatory results. Omega-3 fatty acid supplementation is one of the most well-studied: a meta-analysis of 68 randomized controlled trials found that fish oil supplementation (at doses of 2–4 grams of EPA+DHA per day) significantly reduced CRP, IL-6, and TNF-alpha levels. If you don't eat fatty fish 2–3 times per week, a high-quality fish oil or algae-based omega-3 supplement is a practical bridge. Curcumin, the active compound in turmeric, has been shown in over 100 clinical trials to inhibit NF-kB — a master regulator of inflammatory gene expression — though it must be taken in a bioavailable form (look for supplements formulated with piperine or phospholipid complexes for adequate absorption). Gut health is another major frontier: approximately 70% of your immune system resides in your gut, and a disrupted microbiome (dysbiosis) is directly linked to elevated systemic inflammation. Consuming fermented foods like kimchi, kefir, sauerkraut, and plain Greek yogurt, as well as prebiotic fiber from onions, garlic, asparagus, and oats, supports a diverse microbiome that helps regulate immune responses. A 2021 study in *Cell* by researchers at Stanford found that a high-fermented-food diet increased microbiome diversity and decreased 19 inflammatory proteins over 10 weeks.
Intermittent fasting has emerged as a powerful anti-inflammatory tool supported by growing mechanistic research. During fasting periods, the body activates autophagy — a cellular cleanup process that removes damaged proteins and organelles that can trigger immune activation — and reduces insulin levels, which in turn lowers inflammatory signaling. A 2019 study in *Cell* found that Ramadan-style fasting significantly reduced pro-inflammatory monocytes circulating in the bloodstream. Reducing alcohol consumption is equally important: even moderate drinking has been shown to disrupt the gut lining, increase intestinal permeability (leaky gut), and elevate inflammatory markers — the CDC recommends no more than 1 drink per day for women and 2 for men. Quitting smoking is non-negotiable; cigarette smoke contains thousands of free radicals that trigger a massive and sustained inflammatory response throughout the body, and every year of smoking cessation progressively lowers inflammatory biomarkers. Cold exposure through cold showers or ice baths has shown preliminary evidence of reducing systemic inflammation via activation of the vagus nerve and norepinephrine release. Vitamin D optimization is also critical — over 40% of Americans are vitamin D deficient, and low vitamin D is strongly associated with elevated CRP and increased susceptibility to autoimmune inflammation. Getting 15–30 minutes of midday sun exposure or supplementing with vitamin D3 (1,000–4,000 IU daily) in consultation with your doctor can make a meaningful difference. Finally, reducing exposure to environmental toxins — including BPA from plastics, pesticide residues on non-organic produce, and indoor air pollutants — reduces the chronic low-grade immune activation these compounds trigger at the cellular level.
❓ Frequently Asked Questions
✍️ Final Thoughts: Your Next Step Toward a Less Inflamed Life
Understanding how to reduce inflammation naturally is genuinely one of the most impactful things you can do for your long-term health — not because it addresses one disease, but because it addresses the underlying biological mechanism driving dozens of them simultaneously. The evidence reviewed in this guide points to a clear and encouraging conclusion: the same lifestyle habits that make you feel better day-to-day — eating real food, moving your body, sleeping well, managing stress, caring for your gut — are the very habits that turn down the dial on chronic inflammation at the cellular level. Diet remains the single most powerful lever, with the Mediterranean pattern offering the strongest and most consistent evidence base. But sleep, exercise, stress management, and targeted supplementation are not optional extras — they are essential co-regulators of your immune system. The compounding effect of combining even three or four of these strategies consistently over 8–12 weeks can produce measurable, meaningful changes in your inflammatory biomarkers, your energy levels, your cognitive clarity, and your long-term disease risk. Chronic inflammation did not appear overnight, and it will not vanish overnight — but the arc of recovery bends faster than most people expect when the right inputs are applied consistently.
So what should you do right now? Start small, start today, and start with what feels most manageable. If your diet is your weakest link, commit to one concrete change this week: swap refined cooking oils for extra-virgin olive oil, add a serving of fatty fish to your weekly menu, or cut your daily added sugar intake by half. If sleep is the issue, set a consistent bedtime for the next 14 days and see what happens. If stress is driving your inflammation, download a meditation app tonight and commit to 10 minutes each morning for the next 30 days. Track how you feel. Consider asking your doctor for a high-sensitivity CRP test (hs-CRP) before you begin and again after 12 weeks of lifestyle change — seeing objective data move in the right direction is one of the most powerful motivators you can have. Share this guide with someone you care about who might benefit, and revisit InfoWellHub (infowellhub.com) for more evidence-based health guidance. Your body has an extraordinary capacity to heal — give it the raw materials it needs and get out of the way.
Post a Comment