📌 Table of Contents ⬆

Intermittent Fasting Side Effects: What Happens to Your Body
Picture this: It's day three of your new intermittent fasting routine, and instead of feeling like a glowing wellness influencer, you're lying on the couch with a splitting headache, a growling stomach, and the kind of brain fog that makes answering a simple email feel like solving calculus. Nobody warned you about the intermittent fasting side effects — and suddenly you're wondering if you made a massive mistake. Here's the thing: you didn't. But you absolutely deserved a heads-up. According to a 2023 survey published in Nutrients, over 60% of new intermittent fasters report at least one noticeable side effect during their first two weeks — and most of them almost quit because they thought something was wrong with them. Spoiler: nothing was. Your body was just doing exactly what bodies do when you shake up a decades-old eating pattern. This guide is the honest, no-fluff breakdown of what's actually happening inside you — and what you can do about it.
For more information, see: National Institutes of Health – Intermittent Fasting Research Review, Mayo Clinic – Intermittent Fasting: What to Know
📌 Quick Summary
- Most side effects are temporary: Hunger, headaches, and fatigue typically peak in days 3–5 and resolve within 2 weeks as your body adapts to a new metabolic rhythm.
- Women may experience unique risks: Hormonal disruption is a documented intermittent fasting side effect in women, with some studies showing cortisol and estrogen fluctuations after prolonged fasting windows.
- Hydration is the #1 fix: Up to 75% of early IF symptoms — headaches, irritability, fatigue — are linked to electrolyte loss, not the fast itself, making proper hydration a game-changer.
📊 The Most Common Intermittent Fasting Side Effects (And Why They Happen)
Let's be real: most intermittent fasting guides spend 90% of their time hyping the benefits — weight loss, longevity, insulin sensitivity — and about two paragraphs on the part where you feel like a deflated balloon. So let's flip that. The intermittent fasting side effects you're experiencing aren't random. They're predictable, physiological, and in most cases, completely reversible. When you restrict your eating window — whether you're doing 16:8, 5:2, or OMAD — your body has to make a dramatic metabolic pivot. For most people eating a standard Western diet, your cells have spent years running on glucose from near-constant food intake. Suddenly cutting that supply triggers a cascade: blood sugar drops, cortisol nudges upward to compensate, insulin sensitivity begins shifting, and your hunger hormone ghrelin starts screaming. A 2021 study in the journal *Cell Metabolism* found that ghrelin levels peak sharply during the first three to five days of a new fasting protocol before naturally declining. That's why day three feels like the end of the world, and day ten feels almost manageable.
Here's why this matters beyond just 'feeling hungry': each side effect has a specific biological driver, which means each one also has a specific fix. Headaches during intermittent fasting are most commonly caused by sodium and magnesium loss — when you fast, your kidneys excrete more electrolytes, and that imbalance creates tension headaches that people mistakenly blame on caffeine withdrawal or low blood sugar. Fatigue and brain fog are the result of your brain stubbornly preferring glucose while your body is still weeks away from efficient ketone production. Irritability — yes, being 'hangry' is real — is tied to low blood glucose triggering a mild stress response in the amygdala, the emotional processing center of the brain. And digestive changes, including constipation or an upset stomach, occur because meal timing directly regulates your circadian digestive rhythm. What most people don't realize is that these aren't signs that intermittent fasting is harming them — they're signs that their metabolism is actively changing. The discomfort is the transition.
Hunger Peaks Early
Ghrelin spikes days 1–3, then drops significantly
Brain Fog Is Real
Glucose dips cause focus issues — ketones fix this
Sleep Can Shift
Late fasting windows may disrupt melatonin patterns
| Side Effect | Root Cause | Typical Duration | Severity Rating | Fix |
|---|---|---|---|---|
| Headaches | Electrolyte loss (sodium/magnesium) | Days 1–7 | ⭐⭐⭐☆☆ | Salt water + magnesium supplement |
| Fatigue | Glucose-to-ketone metabolic shift | Days 2–10 | ⭐⭐⭐⭐☆ | Stay active; light walks help |
| Hunger Pangs | Ghrelin hormone spike | Days 1–5 | ⭐⭐⭐⭐⭐ | Black coffee, water, distraction |
| Brain Fog | Low glucose, pre-ketosis state | Days 3–14 | ⭐⭐⭐☆☆ | MCT oil in coffee; stay hydrated |
| Irritability | Blood sugar dip + cortisol rise | Days 1–7 | ⭐⭐⭐☆☆ | Protein-rich first meal; sleep priority |
| Digestive Changes | Disrupted circadian gut rhythm | Days 5–21 | ⭐⭐☆☆☆ | Fiber-rich eating window meals |
💡 Key takeaway: Every major intermittent fasting side effect has a biological explanation — and a practical solution. You're not broken; you're adapting.
🎯 Intermittent Fasting Side Effects in the First Week: A Day-by-Day Breakdown
The intermittent fasting side effects first week is one of the most Googled phrases around this topic — and for good reason. That first seven days is basically a gauntlet, and walking into it blind is why so many people quit before the magic starts. Here's the truth most guides won't tell you: the first week isn't really about weight loss. It's about your body desperately negotiating with a new reality. Your insulin levels are dropping, your liver is beginning to mobilize glycogen stores, and your hunger signals are temporarily in overdrive. A 2020 review in *Obesity Reviews* confirmed that adaptive thermogenesis and hormonal recalibration begin within 48–72 hours of consistent fasting, meaning your body is working harder than it looks. The side effects you feel are proof that the process is working — not proof that it's failing.
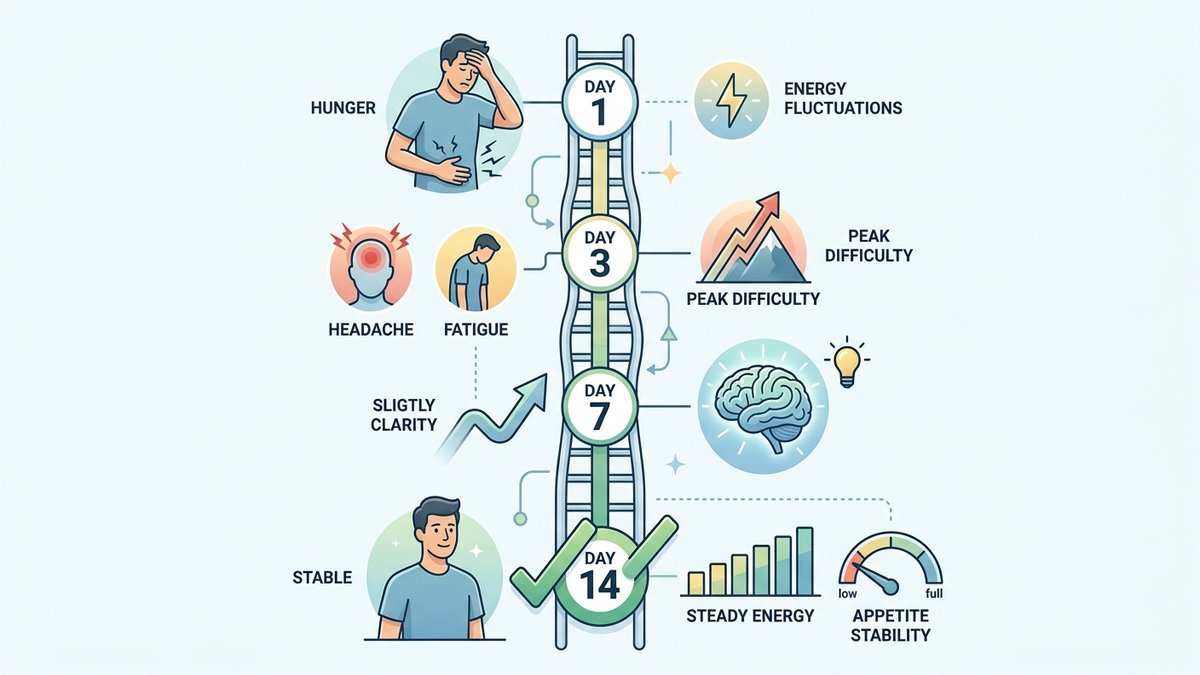
The surprising part? The timeline is remarkably consistent across most people. Days one and two are often the easiest — you're riding motivation and your glycogen stores haven't fully depleted yet. Day three is typically the peak of misery: headaches, hunger, and mood dips converge into what some IF veterans call 'the wall.' By days five through seven, a noticeable shift begins. Hunger windows shorten. Energy starts to stabilize. Many people report their first genuine mental clarity around day six or seven — what some researchers loosely call the 'ketone lift,' when the brain begins efficiently using ketone bodies as fuel. Understanding this timeline transforms the experience from 'I'm failing' to 'I'm exactly on schedule.'
Anticipate Days 3–4 (Don't Quit Here)
Days three and four are physiologically the hardest stretch of any new intermittent fasting protocol, and this is the exact point where most people abandon the plan. Your glycogen stores are largely depleted, ghrelin is at peak production, and your brain hasn't yet adapted to ketone fuel. This is temporary — but it feels permanent. The single best thing you can do here is pre-plan your breaking-fast meal to be high in protein and healthy fats: think eggs with avocado, Greek yogurt with nuts, or a salmon bowl. Protein triggers satiety hormones (leptin and PYY) faster than carbohydrates and blunts that ravenous feeling within 20–30 minutes of eating. Don't use days 3–4 as a signal to quit. Use them as a signal that you're right on track.
Hydrate Strategically, Not Just Abundantly
Drinking 'more water' is good advice. Drinking electrolyte-balanced fluids is great advice. Here's the distinction: plain water during an extended fast can actually dilute your already-depleted sodium and potassium levels, worsening headaches and fatigue rather than fixing them. A simple fix used by experienced fasters is adding a pinch of sea salt and a squeeze of lemon to 16 oz of water each morning during the fast. This replenishes sodium without breaking the fast. Magnesium glycinate at 200–400mg before bed is also widely reported to reduce fasting-related headaches and improve sleep quality during the adaptation phase — and sleep quality during IF week one is notoriously poor without intervention.
Break Your Fast with Purpose, Not Hunger
One of the most overlooked intermittent fasting side effects is what happens when you break your fast poorly. After 16+ hours of fasting, your digestive system is primed but sensitive. Slamming a massive, carbohydrate-heavy meal — say, a stack of pancakes at 11am — triggers a dramatic insulin spike followed by a rapid blood sugar crash, leaving you more fatigued and foggy than before you ate. Studies show that breaking a fast with a moderate-protein, low-glycemic meal produces steadier energy levels and better satiety signaling throughout the eating window. Think of your first meal not as the reward for surviving the fast, but as the foundation for how you'll feel for the next 16 hours.
Track Symptoms Without Judgment
Keeping a simple daily log during your first week — even just notes in your phone — transforms your relationship with intermittent fasting side effects from panic to pattern recognition. Note your hunger level (1–10) at fasting hours 12, 14, and 16. Note your energy and mood at the same intervals. Within three to five days, you'll likely notice that hunger spikes at predictable times (often around when you used to eat), then naturally subsides after 20–30 minutes without intervention. This is ghrelin following your old eating clock — and it resets the more consistently you fast. Seeing this pattern on paper makes it feel manageable rather than miserable. You're training your hunger, not suffering through it.
⚖️ Is Intermittent Fasting Safe for Women? Pros, Cons & What the Research Actually Says
This section deserves its own honest conversation, because is intermittent fasting safe for women is one of the most important — and most frequently glossed-over — questions in the entire IF space. The short answer is: it depends, and the nuance matters enormously. Women's bodies are exquisitely sensitive to caloric and hormonal signals because reproduction is metabolically expensive. When the body senses prolonged energy restriction, it can activate what researchers call 'energy conservation mode,' which may suppress the hypothalamic-pituitary-ovarian (HPO) axis — the hormonal chain that regulates menstrual cycles and fertility. A frequently cited animal study from 2013 in *Endocrinology* showed that female rats on intermittent fasting protocols developed disrupted estrous cycles, elevated cortisol, and signs of hypothalamic stress. Human evidence is more mixed, but several case reports and small clinical studies document menstrual irregularities in women practicing aggressive fasting windows (20+ hours) consistently.
Here's the truth most guides won't tell you: the 16:8 protocol is significantly safer for women than longer fasting windows like 20:4 or extended 24-hour fasts. Multiple studies show that 14–16 hour fasting windows in women can improve insulin sensitivity, support healthy weight loss, and reduce inflammatory markers without disrupting hormonal cycles — particularly when eating windows are centered around midday rather than early morning. The problems tend to arise when women combine aggressive fasting windows with caloric restriction and high-intensity exercise simultaneously. That triple combination dramatically increases cortisol, depletes glycogen, and sends reproductive hormones into suppression. The takeaway? IF can absolutely be safe and beneficial for women — but it requires a gentler, more personalized approach than the one-size-fits-all protocols most internet guides recommend.
Pros
- ✅ Improved insulin sensitivity: Clinical trials show 16:8 IF reduces fasting insulin by up to 31% in both men and women over 8–12 weeks
- ✅ Sustainable weight loss: A 2022 meta-analysis found IF produces comparable or superior fat loss to continuous caloric restriction with less muscle loss
- ✅ Reduced inflammation: CRP (C-reactive protein), a key inflammation marker, drops measurably after 4+ weeks of consistent time-restricted eating
- ✅ Hormonal benefits for men: Testosterone levels show modest increases with 16-hour fasting windows, supporting lean muscle retention
Cons
- ❌ Menstrual disruption risk for women: Aggressive fasting windows (18–24 hrs) may suppress the HPO axis, leading to irregular or absent periods
- ❌ Cortisol elevation: Prolonged fasting spikes cortisol, which can worsen anxiety, disrupt sleep, and promote abdominal fat storage with chronic stress
- ❌ Not recommended during pregnancy or breastfeeding: Caloric and nutrient demands during these phases make fasting physiologically counterproductive and potentially harmful
⚠️ Important: Women who notice missed periods, significant hair loss, extreme fatigue, or worsening anxiety after starting intermittent fasting should shorten their fasting window to 12–14 hours and consult a healthcare provider. These are real intermittent fasting side effects that warrant medical attention, not just 'pushing through.'
✅ How Long Does Intermittent Fasting Hunger Last — And How to Make It Bearable Faster
If there's one question that drives people to Google at 10am on a Tuesday during their fast, it's this one: how long does intermittent fasting hunger last? The honest answer is both encouraging and nuanced. The acute hunger spikes — the gnawing, distract-me-from-everything kind — typically last 20–30 minutes per episode before ghrelin naturally subsides, even without eating. This is well-documented in appetite research: hunger comes in waves, not a straight line. The broader adaptation timeline — where hunger during the fasting window feels genuinely comfortable rather than forced — takes most people two to four weeks of consistent practice. A landmark study in the journal *Obesity* (2020) showed that after 14 days of 16:8 fasting, participants reported a statistically significant reduction in subjective hunger scores and cravings during fasting hours, independent of weight lost. Your hunger isn't permanent. It's a habit — and habits change. The key is surviving the first two weeks without letting a 25-minute ghrelin wave convince you that you're dying. You're not. You're adapting. There's a significant difference. 💡 Pro Tip: Scheduling black coffee or green tea at your peak hunger window (usually 1–2 hours before your eating window opens) is one of the most effective, evidence-backed appetite suppression strategies for intermittent fasters. Both caffeine and EGCG in green tea blunt ghrelin signaling measurably.
Beyond the hunger question, there are a handful of other time-restricted eating adverse effects worth understanding — particularly ones that tend to sneak up in weeks two through four, after the dramatic first-week symptoms have faded. Sleep disruption is one. If your eating window extends late into the evening (say, noon to 8pm), late-night meals can delay melatonin onset and fragment sleep, which paradoxically increases hunger hormones the next day through a cortisol-ghrelin feedback loop. Shifting your eating window earlier — 10am to 6pm, for example — tends to produce better sleep outcomes and smoother morning fasts. Hair shedding (telogen effluvium) can appear four to eight weeks into IF, particularly when overall caloric intake has dropped significantly. This isn't unique to fasting — it's a stress response your hair follicles mount in response to rapid dietary change — and it's typically temporary and self-resolving. ⚡ Quick Fact: Ensuring your eating window includes adequate biotin, iron, and protein (at least 0.7g per pound of bodyweight) is the most effective way to prevent fasting-related hair loss. ✅ Your IF Symptom Checklist: Track hunger (wave-based, not constant? ✅ Normal), energy crashes (post 5pm? ✅ Adjust meal timing), headaches (daily before noon? ✅ Add electrolytes), mood dips (days 2–5 only? ✅ Normal adaptation), sleep issues (eating past 7pm? ✅ Shift window earlier).
❓ Frequently Asked Questions
✍️ Final Thoughts: Your Next Step With Intermittent Fasting
If you've read this far, you're already ahead of 90% of people who start intermittent fasting blindly, hit a wall on day three, and assume they're doing it wrong. Here's what I want you to walk away with: intermittent fasting side effects are not failure signals — they are transition signals. Every headache, every hunger wave, every foggy Tuesday morning is your metabolism renegotiating its operating system. That's not comfortable. But it is meaningful. The data backs this up: studies consistently show that people who push through the first two weeks report dramatically better hunger control, improved energy, and real metabolic benefits by week four. The side effects are front-loaded precisely because the benefits take time to materialize — and most people quit right before the curve turns. Women deserve special mention here: if your body is sending strong signals — missed periods, worsening anxiety, persistent exhaustion — those signals matter. Shorten your window. Eat more within it. There is no version of intermittent fasting worth your hormonal health. The protocol should serve your life, not demand sacrifice from it.
Here's what I'd do if I were starting today: First, start with a 12-hour fast and add one hour every three days until you reach your target window — this gradual approach cuts first-week side effects significantly. Second, buy magnesium glycinate and sea salt before day one — electrolyte management is the single highest-ROI move for surviving the adaptation phase comfortably. Third, log your hunger and energy for the first 14 days — not obsessively, just a quick phone note. Patterns will emerge that make the whole process feel like science rather than suffering. And finally, give it four full weeks before you evaluate whether it's working. One week is not enough data. Two weeks is barely enough. Four weeks is when the real story starts to show up in your energy levels, your hunger patterns, and yes — your body composition. You've now got the complete picture of intermittent fasting side effects: what causes them, how long they last, who should be cautious, and exactly what to do about each one. The only thing left is to start — thoughtfully, with realistic expectations and a solid pinch of sea salt in your water bottle. You've got this. 💪
Post a Comment