📌 Table of Contents ⬆

Vitamin D Deficiency Symptoms: 12 Warning Signs You Shouldn't Ignore
Picture this: you've been exhausted for months, your bones ache for no obvious reason, and you keep catching every cold that goes around the office — yet every doctor visit comes back 'normal.' Sound familiar? You might be experiencing vitamin d deficiency symptoms, one of the most overlooked health issues in America today. Here's the jaw-dropping part: nearly 42% of American adults are vitamin D deficient, according to research published in the journal Nutrition Research — and most of them have absolutely no idea. This post breaks down all 12 warning signs you need to know, so you can stop guessing and start feeling like yourself again.
For more information, see: National Institutes of Health — Vitamin D Fact Sheet, Mayo Clinic — Vitamin D Deficiency
📌 Quick Summary
- Fatigue is the #1 overlooked sign: Studies show that people with vitamin D blood levels below 20 ng/mL report significantly higher fatigue scores than those with optimal levels.
- Bone pain often goes misdiagnosed: Low vitamin D directly impairs calcium absorption, causing bone density loss that many doctors initially attribute to aging or arthritis.
- Getting tested is simple and cheap: A basic 25-hydroxyvitamin D blood test costs as little as $30–$50 and gives you a definitive answer within days.
📊 Why Vitamin D Deficiency Symptoms Are So Easy to Miss
Here's the frustrating truth most guides won't tell you: vitamin d deficiency symptoms don't show up overnight, and they don't announce themselves with a neon sign. They creep in slowly — a little more tiredness here, a little more brain fog there — until one day you realize you haven't felt truly well in years. That gradual onset is exactly why over 1 billion people worldwide are estimated to have insufficient vitamin D levels, according to the World Health Organization. Your body needs vitamin D for literally hundreds of biological processes, from regulating immune function to keeping your bones strong and your mood stable. When levels drop, every single one of those processes takes a hit. The sneaky part? Many of these symptoms overlap with other common conditions like hypothyroidism, depression, or chronic fatigue syndrome — which is why vitamin D is frequently the last thing anyone checks.
What most people don't realize is that vitamin D isn't technically a vitamin at all — it's a hormone. Your skin produces it when exposed to UVB sunlight, which means that anything blocking that exposure (living in northern states, working indoors, using sunscreen religiously, or having darker skin) dramatically raises your deficiency risk. A landmark study published in the *Archives of Internal Medicine* found that 77% of Americans don't get enough vitamin D when measured against optimal — not just minimum — health thresholds. The surprising part? Even people who live in sunny climates can be deficient if they spend most of their time indoors or heavily covered. Understanding this context is key to recognizing why these low vitamin d signs are so widespread and why you shouldn't dismiss any of the 12 warning signs we're about to walk through.
Chronic Fatigue
Persistent tiredness that sleep simply can't fix
Bone & Back Pain
Dull aches linked directly to calcium loss
Frequent Illness
Low D weakens your immune defense fast
| Warning Sign | How Common | Often Mistaken For | Severity if Ignored | Urgency Rating |
|---|---|---|---|---|
| Chronic Fatigue | Very Common | Poor sleep / stress | High | ⭐⭐⭐⭐⭐ |
| Bone & Back Pain | Common | Arthritis / aging | Very High | ⭐⭐⭐⭐⭐ |
| Frequent Infections | Common | Weak immune system (general) | High | ⭐⭐⭐⭐ |
| Depression & Mood Changes | Moderately Common | Clinical depression | High | ⭐⭐⭐⭐ |
| Hair Loss | Less Common | Stress / genetics | Moderate | ⭐⭐⭐ |
| Slow Wound Healing | Less Common | Circulation issues | High | ⭐⭐⭐⭐ |
| Muscle Pain | Common | Fibromyalgia / overexertion | Moderate | ⭐⭐⭐⭐ |
| Brain Fog | Common | Anxiety / burnout | Moderate | ⭐⭐⭐ |
💡 Key takeaway: Most vitamin D deficiency symptoms mimic other conditions, which is exactly why a blood test — not symptom-guessing — should always be your first move.
🎯 The 12 Vitamin D Deficiency Symptoms You Shouldn't Ignore
Alright, let's get into it — the actual list. These 12 vitamin d deficiency symptoms are ranked not by severity alone, but by how frequently they're dismissed or misattributed. If you're nodding along to more than three of these, that's your body sending you a very specific message. The good news? Vitamin D deficiency is one of the most correctable nutritional issues in modern medicine. But you have to know what you're looking for first. Each symptom below has a real biological mechanism behind it — this isn't vague wellness talk, it's physiology. Signs of low vitamin d in women, in particular, can be especially subtle and hormonally intertwined, which is why we've flagged gender-specific nuances where they exist.
One more thing before we dive in: experiencing one or two of these symptoms doesn't automatically mean you're deficient. But if you're stacking three, four, or five of them — especially alongside risk factors like limited sun exposure, a plant-based diet, or being over 65 — then you owe it to yourself to get tested. How do you know if you have vitamin d deficiency for certain? A 25-hydroxyvitamin D blood test is the gold standard. Anything below 20 ng/mL is classified as deficient by the National Institutes of Health. Levels between 20–29 ng/mL are considered insufficient. Optimal health typically requires 40–60 ng/mL. Keep that in mind as you read through this list.
1. Recognize Persistent, Unexplained Fatigue
This is the big one — and the most commonly dismissed. Vitamin d deficiency symptoms fatigue and bone pain often travel together, but fatigue alone can be a standalone red flag. A 2015 study published in the *North American Journal of Medical Sciences* found a direct correlation between low serum vitamin D levels and reported fatigue severity in otherwise healthy adults. Your cells rely on vitamin D to produce energy efficiently at the mitochondrial level. When D is low, that energy production becomes sluggish — no matter how many hours of sleep you get. If you're sleeping 8 hours and waking up exhausted, and coffee barely touches it, low vitamin D should absolutely be on your radar. This isn't 'you just need to exercise more' fatigue. It's deep, cellular, won't-quit fatigue that shows up every single day.
2. Notice Bone Pain and Lower Back Aches
Vitamin D is essential for calcium absorption in the gut. Without adequate D, your body literally cannot pull enough calcium from the food you eat — so it starts borrowing from your bones. Over time, this leads to a condition called osteomalacia (soft bones in adults), which presents as dull, aching bone pain, especially in the lower back, hips, legs, and ribs. This is distinct from the sharp, localized pain of a fracture — it's more of a widespread achiness that feels worse at night or after sitting for long periods. Signs of low vitamin d in women are particularly pronounced here because women already have a higher baseline risk for bone density loss, especially post-menopause. If you've been told you have 'non-specific back pain' and nothing structural shows up on imaging, please ask your doctor about a vitamin D test.
3. Watch for Frequent Colds, Flu, and Infections
Your immune system is essentially vitamin D's playground. Vitamin D receptors are found on virtually every immune cell in your body — T cells, B cells, macrophages — and D directly modulates how aggressively those cells respond to pathogens. A landmark meta-analysis published in the *BMJ* in 2017 analyzed 25 randomized controlled trials and found that vitamin D supplementation significantly reduced the risk of acute respiratory infections, particularly in people who were severely deficient. If you're the person in the office who catches every bug that goes around, or if you've had more than three respiratory infections in a single year, low vitamin D might be the immune system gap you didn't know you had. This is especially critical during winter months when UVB exposure plummets across most of the United States.
4. Pay Attention to Mood Changes and Depression
Here's one that surprises a lot of people: vitamin D plays a direct role in serotonin synthesis — the neurotransmitter most closely linked to mood regulation. Vitamin D receptors are densely packed in the same regions of the brain that regulate mood, including the prefrontal cortex, hippocampus, and hypothalamus. Multiple studies have found a significant association between low vitamin D levels and depressive symptoms, particularly seasonal affective disorder (SAD), which spikes in the darker winter months. A 2020 meta-analysis in the *Journal of Affective Disorders* found that vitamin D supplementation had a measurable antidepressant effect in people with clinical depression who were also deficient. If you've noticed that your mood tanks every winter, or that you feel a persistent low-grade sadness you can't shake, low vitamin D signs could be a contributing factor worth investigating alongside professional mental health support.
⚖️ Getting Tested vs. Self-Supplementing: What You Really Need to Know
This is where a lot of people make a well-intentioned mistake. They read about vitamin d deficiency symptoms, recognize themselves in the list, and immediately run to the pharmacy to grab the biggest vitamin D supplement they can find. And while the instinct is completely understandable, it's actually skipping a critical step. Vitamin D toxicity is real — it's called hypervitaminosis D, and it happens when blood calcium levels rise too high due to excessive supplementation. Symptoms include nausea, weakness, frequent urination, kidney stones, and in severe cases, cardiac arrhythmia. The NIH notes that toxicity is almost always the result of supplementation, not sun exposure or diet, because your skin has a self-regulating mechanism that prevents overproduction. The takeaway? Get tested first, then supplement based on your actual numbers — not your guessed-at deficiency.
That said, if getting a blood test immediately isn't possible for you, there are some smart, low-risk steps you can take in the meantime. Spending 15–20 minutes in direct midday sun (arms and legs exposed, without sunscreen) several times a week is genuinely helpful for most light-skinned adults. Foods like fatty fish (salmon, mackerel), egg yolks, and fortified dairy or plant milks provide modest amounts of dietary vitamin D. And if you do choose to supplement before testing, most integrative medicine doctors consider 1,000–2,000 IU daily to be a safe starting point for most adults — but please confirm this with your own healthcare provider, because context matters enormously. Your weight, your baseline levels, your medications, and your overall health picture all factor into the right dose for you.
Pros
- ✅ Pro 1 — Getting Tested: Gives you an exact baseline number so supplementation is precise, not guesswork — no risk of over-correcting.
- ✅ Pro 2 — Sun Exposure: Free, natural, boosts mood via serotonin simultaneously, and comes with zero toxicity risk.
- ✅ Pro 3 — Dietary Sources: Adds vitamin D alongside other nutrients (omega-3s from fish, protein from eggs) for a whole-food synergy.
- ✅ Pro 4 — Supplementing Correctly: When guided by test results, D3 supplements are highly effective — studies show they raise serum levels faster than D2.
Cons
- ❌ Con 1 — Supplementing Without Testing: Risk of hypervitaminosis D with very high doses; impossible to know if you're correcting deficiency or creating toxicity.
- ❌ Con 2 — Relying on Sun Alone: Impractical for people in northern states (above 37° latitude) from October through March — UVB simply isn't strong enough.
- ❌ Con 3 — Diet Alone: Very difficult to reach sufficient levels through food; even a salmon-rich diet provides only about 400–600 IU per serving, often not enough to correct a true deficiency.
⚠️ Important: Always request a 25-hydroxyvitamin D [25(OH)D] test specifically — not just a general vitamin panel. This is the only test that accurately reflects your body's vitamin D status. Ask your doctor to include it at your next annual checkup.
✅ 8 More Vitamin D Deficiency Symptoms That Fly Under the Radar
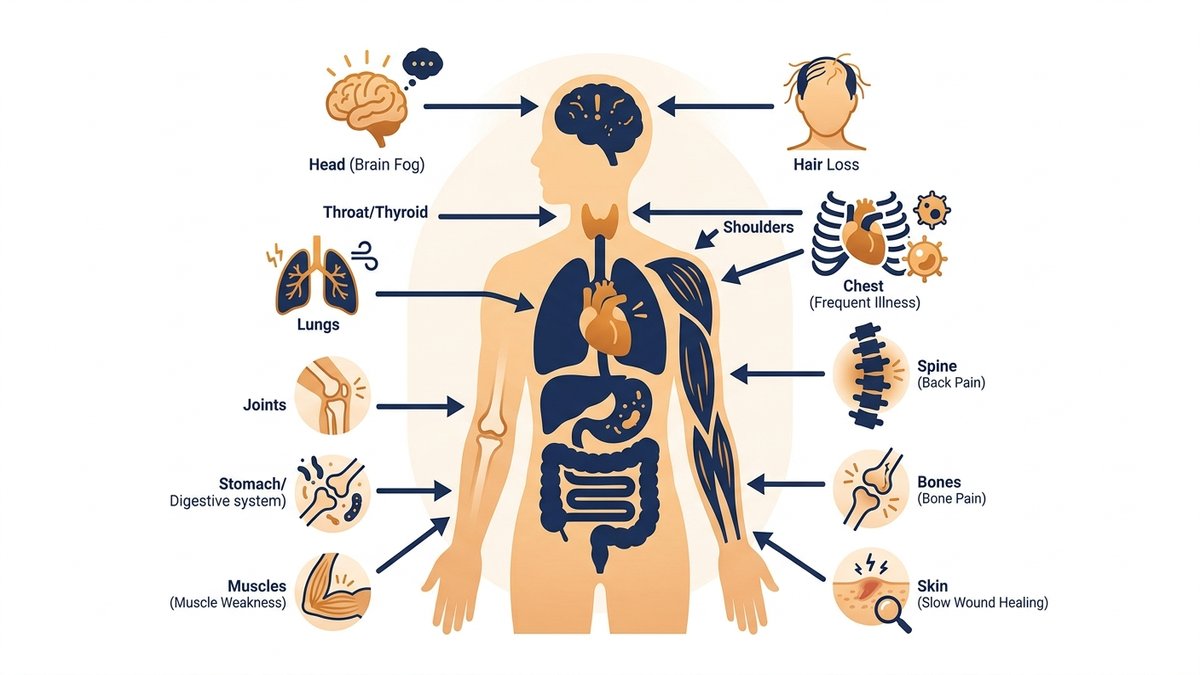
We covered the big four above — fatigue, bone pain, frequent illness, and mood changes. But vitamin d deficiency symptoms don't stop there. Here are eight more low vitamin d signs that are frequently missed, dismissed, or chalked up to 'just getting older.' Hair loss is one of the more surprising ones: vitamin D plays a role in the hair follicle cycle, and a deficiency has been linked to alopecia areata (an autoimmune hair loss condition) in multiple studies. Slow wound healing is another — D is critical to the production of compounds that form new skin, so cuts and scrapes that seem to heal unusually slowly can be a quiet red flag. Muscle weakness and pain often get labeled as fibromyalgia or general deconditioning, but research has repeatedly shown that correcting vitamin D deficiency significantly reduces muscle pain scores. And brain fog — that maddening inability to concentrate or recall words — has been associated with low D levels through its role in neurological function and inflammation regulation.
The remaining four are worth a quick but serious mention. Unexplained weight gain has been linked to vitamin D deficiency through its effect on leptin (the hunger hormone) and fat cell regulation — though more research is ongoing. Sweating excessively from the head was historically one of the first signs pediatricians looked for in rickets (the childhood form of vitamin D deficiency) and still appears in some adults. Gut health issues, particularly those involving fat malabsorption (like Crohn's disease or celiac disease), can both cause and be worsened by vitamin D deficiency, since D is a fat-soluble vitamin. And finally — this one genuinely surprises people — high blood pressure. Vitamin D helps regulate the renin-angiotensin system, which controls blood pressure. A major review published in *Hypertension* found that vitamin D deficiency was associated with a 35% higher risk of hypertension. If you're stacking several of these alongside the core four symptoms, please don't wait. Get the test.
❓ Frequently Asked Questions
✍️ Final Thoughts: Your Next Step Starts Today
If you've read this far, you're already ahead of the 42% of American adults who are quietly deficient and don't even know it. Vitamin d deficiency symptoms are maddeningly easy to dismiss — fatigue, mood dips, achy bones, frequent colds — because they look exactly like the symptoms of a busy, stressed, modern life. And that's precisely what makes them so dangerous to ignore. The real cost of untreated vitamin D deficiency isn't just feeling tired. It's accelerating bone loss, suppressed immunity, neurological decline, and cardiovascular risk compounding quietly over years. The good news — genuinely, sincerely — is that this is one of the most correctable nutrient deficiencies in existence. A simple blood test, a conversation with your doctor, and a targeted supplement protocol can turn this around faster than you'd expect. You don't have to white-knuckle through exhaustion and achiness thinking that's just how life feels now. It doesn't have to be.
Here's what I'd do if I were in your position right now — three concrete steps, starting today. First, call your doctor or visit a lab (many offer direct-to-consumer testing) and request a 25-hydroxyvitamin D blood test. Write it down, say it out loud, don't leave that appointment without it. Second, in the meantime, try to get 15–20 minutes of midday sun exposure on your arms and legs at least 3–4 times per week — it's free, it works, and it'll boost your mood while you wait for results. Third, take a look at your diet and consider adding more fatty fish, fortified foods, and eggs as easy dietary sources. Once you have your test results, work with a healthcare provider to dial in the right supplementation dose for your specific level. And if you want to go deeper on related nutrient gaps that often travel alongside vitamin D deficiency — magnesium and vitamin K2 are the big ones — check out our related posts right here on InfoWellHub. Your energy, your bones, your immune system, and your mood are all waiting on the other side of this one blood test. Go get it.
Post a Comment